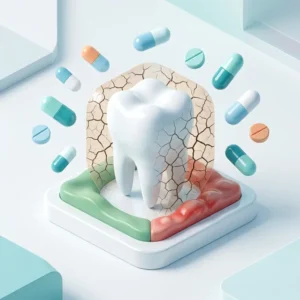
Many commonly prescribed drugs can harm oral health by reducing saliva and altering gum tissues. Medications such as antihistamines, antidepressants, anticholinergics, and opioids often cause xerostomia (dry mouth), leading to higher rates of cavities and periodontal disease. Other drugs (e.g. calcium channel blockers, phenytoin, cyclosporine) can cause gum overgrowth, and inhaled steroids or chemotherapy drugs can predispose to oral infections like thrush. Patients on these medications may notice symptoms like dry, cracked lips, burning or sticky mouth, bleeding or swollen gums, and a tendency for tooth decay. Dental management focuses on hydration, meticulous hygiene, topical fluoride, saliva substitutes, and coordinating with physicians to adjust medications if needed. In Petersburg, VA, our Southside Dental Cares team works with patients to strengthen fluoride defenses (our water is fluoridated ~0.7 ppm) and provide professional gum care and cavity prevention. The sections below review causes, common drug classes, clinical approaches, and local preventive strategies, with evidence from NIH, ADA, and peer-reviewed sources.
Causes and Mechanisms of Medication-Induced Oral Effects
Medication side effects can directly disrupt oral tissues and saliva, creating a cascade of problems:
Xerostomia (Dry Mouth): Many medications have anticholinergic effects that inhibit salivary glands. Examples include diphenhydramine (antihistamine), oxybutynin (for bladder), SSRIs/SNRIs (antidepressants), opioids, and benzodiazepines. As a result, patients feel persistent dryness, find their mouth sticky, and may have trouble swallowing or speaking. For instance, tricyclic antidepressants can reduce parotid salivary flow by ~58%, while common SSRIs reduce it ~32%. Reduced saliva impairs natural buffering of acids; without enough spit, the risk of dental caries and periodontal disease rises sharply. Patients often compensate with sugary candies or drinks, further acidifying the mouth. Management of xerostomia (hydration, saliva stimulants) is discussed below.
Figure: Medications that reduce saliva can leave patients with a parched, uncomfortable mouth, a condition called xerostomia.
Medication-Related Gingivitis and Periodontal Disease: Medication-induced dry mouth alone increases plaque accumulation and gum inflammation. In addition, certain drug classes directly alter gum tissue. Notably, calcium channel blockers (e.g. nifedipine, verapamil) can cause gingival hyperplasia – an overgrowth of gum tissue – in up to 83% of patients on high doses. Antiepileptic phenytoin causes similar gum overgrowth (roughly 40–50% of long-term users). Immunosuppressants like cyclosporine and high-dose steroids also promote gingival enlargement and candidiasis. The combined effect is red, swollen gums that bleed easily (gingivitis) and can progress to periodontitis if unchecked. (Gingivitis is reversible with treatment; periodontitis can cause irreversible bone and tissue loss.)
Figure: Inflamed, bleeding gums (gingivitis) – a common sign of periodontal disease. Reduced saliva and medication-induced tissue changes (see Gum Care) can precipitate or worsen gingivitis, a leading cause of adult tooth loss.
Dental Caries (Cavities) and Enamel Erosion: Medications can raise cavity risk via several pathways. Dry mouth means less saliva to neutralize acids and repair enamel, so cavities become more likely. Patients may frequently sip sugary drinks or chew candy to ease dry mouth, fueling more acid production by plaque bacteria. Some drugs indirectly contribute to enamel erosion: for example, nausea from chemotherapy or reflux from corticosteroids and opioids can expose teeth to stomach acid. Over time, enamel thinning and cavity formation (especially on roots or in grooves) accelerate. Preventing caries requires robust fluoride protection (see Prevention below) and dietary counseling to avoid frequent sugars.
Oral Candidiasis (Thrush): Medications that lower immunity or disturb oral flora can trigger Candida albicans overgrowth. Inhaled corticosteroids (for asthma/COPD) are classic culprits: up to 20% of ICS users develop oropharyngeal candidiasis. Cancer chemotherapy also suppresses immune defenses and irritates mucosa, making thrush (white, curd-like patches) common in those patients. Patients with thrush may notice creamy plaques on their tongue, palate or cheeks and a cottony or burning sensation. Gentle rinsing after inhaler use can reduce steroid residue and infection risk. If thrush occurs, topical antifungals (nystatin or clotrimazole) are typically needed.
Figure: Oral thrush (candidiasis) presents as white, curd-like patches. It is often seen in patients using steroid inhalers or immunosuppressants. Good oral hygiene and rinsing after inhalers help prevent thrush, and topical antifungals can treat it.
Taste and Smell Changes: Some drugs alter taste receptors or salivary composition. ACE inhibitors (e.g. captopril) are known for metallic taste and dry cough, and many hypertensives and antibiotics can cause dysgeusia (reduced taste). Patients may describe foods tasting bland or bitter. Loss of taste can diminish appetite or lead to excessive seasoning, impacting nutrition. These effects are usually reversible after changing the medication or discontinuing it under a doctor’s guidance.
Common Drug Classes and Their Oral Effects
| Drug Class (Examples) | Key Oral Side Effects | Relative Prevalence (Notes) | Management Strategies |
| Antidepressants (SSRIs, TCAs) | Dry mouth, burning mouth, ↑caries, candidiasis | Dry mouth in ~30% (SSRIs)–50% (TCAs); elevated caries risk. | Stay hydrated, sugar-free gum or lozenges. High-strength fluoride toothpaste/rinses (see cavity prevention). Regular dental check-ups for cleanings and fluoride varnish. |
| Antihypertensives<br>(ACEi, ARBs, β-blockers, Ca-channel blockers, diuretics) | Dry mouth; gingival enlargement (esp. Ca-blockers); taste changes; lichenoid reactions (beta-blockers, ACEi) | Most classes cause some xerostomia. Calcium-channel blockers (e.g. nifedipine) cause gum overgrowth in 2–83% of users. ACE inhibitors can cause altered taste or ulceration. | Encourage water, saliva substitutes. For Ca-blockers, meticulous hygiene to limit hyperplasia; consider alternative medication with prescribing physician if severe. Use topical fluoride and antihypertensive-friendly dental analgesics. |
| Antihistamines & Anticholinergics (diphenhydramine, oxybutynin, ipratropium) | Dry mouth (xerostomia); thickened secretions; sedation (antihistamines) | Very common – >40% experience dry mouth on first-generation antihistamines; >50% on anticholinergic urinary or allergy meds. | Sip water frequently; saliva substitutes or sipping sugar-free candy. If possible, use non-sedating antihistamines or adjust dosing schedule. |
| Opioids (morphine, codeine, tramadol) | Dry mouth; decreased salivary flow; glossodynia (tongue pain); sedation | Widespread use: chronic users have reduced saliva and higher caries. Long-term opioid users show much higher rates of missing teeth. | Encourage hydration; chew sugarless gum (xylitol) to stimulate saliva. Limit sedating use at night. Discuss alternative analgesics or adjunct therapies with provider. |
| Chemotherapy Agents (5-FU, anthracyclines, bisphosphonates for cancer) | Mucositis (painful ulcers), xerostomia, taste changes, candidiasis, increased caries | Oral mucositis affects >40–80% of chemo patients. Dry mouth and infections (bacterial, fungal) are very common. | Pre-treatment dental exam; gentle dental care during chemo; use saliva substitutes. Antimicrobial mouth rinses (baking soda or chlorhexidine) for mucositis. Treat thrush or ulcers promptly. Coordinate care with oncologist. |
| Bisphosphonates/Denosumab (alendronate, zoledronic acid) | Medication-related osteonecrosis of jaw (MRONJ), mucosal pain | Rare in osteoporosis doses (<1%), higher (1–10%) in cancer regimens. Risk increases with >2 years use. | Maintain excellent oral hygiene and regular dental visits to minimize infection risk. Avoid extractions/invasive procedures if possible; if needed, coordinate with physician. Brief “drug holiday” may be recommended by specialists. |
| Immunosuppressants (cyclosporine, methotrexate, corticosteroids) | Gingival hyperplasia (cyclosporine ~25–30% of pts); candidiasis; delayed healing; oral ulcers | ~30% of cyclosporine users get gum overgrowth. High-dose steroids (for asthma, arthritis) cause frequent thrush and delayed wound healing. | Intensify plaque control (brushing/flossing). Rinse mouth after steroid inhalers; use spacer. Topical antifungals for candidiasis. Discuss drug alternatives or dose reduction with physician if gum overgrowth is severe. |
| Antiepileptics (phenytoin, carbamazepine) | Gingival hyperplasia (gingival enlargement); dry mouth (rare) | Phenytoin causes gingival overgrowth in ~40–50% of patients. Carbamazepine and others have lower rates. | Rigorous oral hygiene and frequent dental cleanings; possible surgical reduction of gum tissue if needed. Neurologist may consider switching drug if oral overgrowth is problematic. |
| Inhaled Corticosteroids (fluticasone, prednisone inhaler) | Oral candidiasis (thrush), dysphonia, cough; possible mucosal atrophy | Up to 10–20% may develop thrush without preventive rinsing; incidence depends on dose and inhaler type. | Rinse mouth thoroughly after each dose or use a spacer device. Consider intermittent oral antifungal prophylaxis if recurrent thrush. Ensure regular dental exams to monitor mucosal health. |
Table: Common drug classes, their typical oral side effects, how often they occur (where known), and key management strategies to mitigate problems. (Sources: ADA clinical guidance, NIH/Aust Prescriber data, and cancer/ADA resources.)
Clinical Signs, Diagnosis, and Management
Clinical Signs and Diagnosis
Patients with medication-induced oral side effects often present with characteristic symptoms and exam findings:
- Dry mouth symptoms: Patients report a constant feeling of “cotton mouth,” difficulty swallowing, cracking at lip corners, or a burning sensation on the tongue. Dentures may become loose. On exam, the mouth may appear dry, sticky, and the tongue may look fissured or reddened. Dentists can measure salivary flow (sialometry) or perform the “chewing-stimulated spit” test if needed.
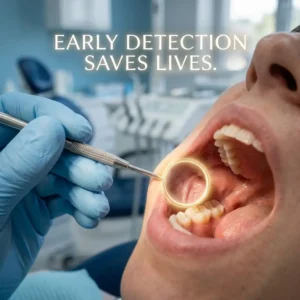
- Gingival changes: Look for inflamed, bleeding, or overgrown gums. As ADA’s MouthHealthy notes, early gingivitis causes gums to turn red and bleed easily. A history of medication use is crucial: ask if the patient is on drugs like calcium blockers, phenytoin, or cyclosporine (all of which the ADA flags for hyperplasia). Chart any gum pockets or recession, and note if oral hygiene seems inadequate (dry mouth often makes brushing painful or less effective).
- Caries and enamel erosion: Closely inspect teeth for new cavities, root caries, or shiny “thinning” of enamel (erosion). Patients with hyposalivation may show rapid new decay, especially on cervical (neck) areas of teeth or between teeth. Dietary history (frequent sips of soda or juices) can confirm acid exposure.
- Oral lesions: Check for candidiasis (white patches that wipe off, often on buccal mucosa or tongue) and dental mucositis (ulcerations) in chemo patients. Also note any lichenoid (white) streaks in mouth potentially from drug reactions (e.g. with antihypertensives or antimalarials).
- Medical/dental history: Review all current medications (prescription, OTC, supplements). Studies show that disclosure of drug lists is often incomplete, so explicitly ask about common offenders (antihistamines, antidepressants, etc). Query systemic conditions (diabetes, Sjögren’s) that may mimic drug effects. If a medication seems implicated, consider consultation with the prescribing physician.
Management Strategies
Oral side effects from medications are managed with both preventive and therapeutic measures:
- Optimize oral hygiene: Emphasize gentle but thorough brushing twice daily and daily flossing (see [Gum Care services] for technique). The Southside Dental team often recommends “water flossers” or interdental brushes if manual flossing is hard. Frequent professional cleanings are key to remove plaque that causes gingivitis. For children or at-risk adults, dental sealants can block grooves where acids concentrate.
- Fluoride and remineralization: Saliva normally supplies minerals to enamel, so with reduced saliva we compensate with fluoride. Use high-strength fluoride toothpaste or gels and consider in-office fluoride varnish applications. ADA guidelines recommend topical fluoride and casein-calcium-phosphate products (CPP-ACP) to rebuild enamel in dry-mouth patients. Patients should ‘spit but not rinse’ after fluoride application to maximize retention.
- Hydration and saliva substitutes: Encourage frequent sipping of water or sugar-free drinks throughout the day to keep tissues wet. Biotene® and other over-the-counter saliva substitutes (gels and sprays) can provide relief. Chewing sugarless gum or xylitol gum stimulates saliva flow. (Caution: people who chew gum too often may increase acid exposure, so limit to recommended 15–20 minutes as needed.) Avoid caffeine, alcohol, and tobacco as they further dry the mouth.
- Dietary counseling: Advise avoiding frequent snacking on sugars or acidic foods/drinks. The [Cavity Prevention] page recommends twice-daily brushing with fluoride toothpaste and limiting sugary/acidic intake. In particular, patients with dry mouth should steer clear of sugary breath mints or cough drops; sugar-free alternatives are better. A diet rich in crunchy vegetables and high in water content can help clean teeth naturally and promote saliva flow.
- Medication review: If severe dry mouth or tissue changes persist, coordinate with the patient’s physician. Some side effects can be mitigated by switching to an alternative drug or adjusting the dose. For example, if gingival hyperplasia from a calcium blocker is problematic, a doctor might change to a different antihypertensive class. Never advise patients to stop a prescribed medication on their own – rather, encourage discussing options with their healthcare provider.
- Topical therapies: For acute symptoms, saliva-stimulating lozenges (pilocarpine or cevimeline) may be prescribed in resistant cases (by a physician). Antimicrobial mouth rinses (e.g., chlorhexidine) can temporarily reduce plaque if brushing is painful. For patients with thrush, topical antifungals (nystatin suspension or clotrimazole troches) are used until infection clears.
- Referral and monitoring: In extreme cases of hyposalivation, a referral to an oral medicine specialist or ENT may be warranted. Patients on high-risk medications (bisphosphonates, high-dose chemo) need more frequent dental follow-ups and possibly preventive antibiotics for invasive procedures. At each visit, re-evaluate medications and counsel on any new drugs that could affect the mouth.
Medication-Induced Oral Health Protocol
Path A: Primarily Dry Mouth
Advise hydration, saliva substitutes, and sugar-free gum.
Path B: Inflamed Gums
Focus on improved brushing/flossing and professional cleaning.
YES (Symptoms Persist)
Action: Review medications with the patient’s Physician (MD).
Check for infections:
- If Thrush: Start antifungal rinses (nystatin, etc.).
- If No Infection: Consider medication change or dose adjustment.
NO (Symptoms Resolved)
Action: Continue monitoring with routine care and maintain regular dental check-ups.
Figure (Mermaid flowchart): Clinical decision pathway for suspected medication-induced dry mouth or gingivitis. Early measures include hydration and improved oral hygiene. If symptoms persist, collaborate with the medical provider on medication review, and treat complications like candidiasis as indicated.
Prevention and Patient Counseling (Petersburg, VA)
Preventive strategies are essential, especially in our Petersburg community. Key points for patients and providers here include:
- Local fluoride programs: Petersburg’s water supply is community-fluoridated at about 0.7 mg/L, the CDC-recommended level. Fluoridation reduces tooth decay by ~25% in children. We remind patients to drink tap water (no need for special supplements) and to brush with fluoride toothpaste to take full advantage of this local public health measure.
- Regular dental visits: Encourage visits every 6 months (or sooner if problems arise). Our Southside Dental Cares clinic in Petersburg provides comprehensive preventive care – for example, professional cleanings, fluoride varnishes, and sealants – tailored to patients with dry mouth and gum issues. Early intervention (such as deep cleaning) can reverse gingivitis before it progresses. The [Gum Care] and [Cavity Prevention] pages detail the services we offer for long-term health.
- Hydration and climate considerations: Petersburg’s hot, humid summers can lead to dehydration; remind patients to increase water intake when outdoors. In winter, indoor heating may dry the air and mouth; using a humidifier at night can help. Patients should avoid mouth breathing (which dries tissue) and consider sugar-free lozenges to stimulate saliva during dry months.
- Lifestyle counseling: Advise against tobacco, vaping, or heavy alcohol use, as these worsen dry mouth and gum disease. Patients prone to seasonal allergies (using OTC antihistamines) should choose non-drying formulations if possible. Dietitians and local clinics (e.g. the Crater District Health Department) can provide resources on nutrition and smoking cessation in Petersburg.
- Local resources: The Virginia Department of Health’s Crater Health District (which covers Petersburg) offers general health clinics and can guide low-income patients to dental care programs. The Greater Richmond & Petersburg Oral Health Alliance works to improve community oral health, and they run events and school sealant programs that Petersburg families can join. When counseling patients, mention these community resources and any upcoming “free dental day” events (often announced by Southside Dental on social media).
- Personalized risk counseling: For Petersburg seniors and those on multiple medications, we emphasize the compounded risk of dry mouth from polypharmacy. We review all medications at dental visits and educate patients about which drugs are likely culprits. Written handouts (in English and Spanish) on managing dry mouth are provided. If a patient is prescribed a new medication known to dry the mouth (e.g. starting a blood pressure pill), our staff proactively reinforces daily fluoride use and saliva substitutes.
Evidence-Based Insights
The links between medications and oral health are well-documented in recent literature and public health reports. The NIH/NIDCR “Oral Health in America” report highlights that psychiatric and pain medications (e.g. antidepressants, antipsychotics, opioids) often compromise saliva and hygiene, contributing to tooth decay and tooth loss. FDA guidelines warn about rare but serious effects like jaw osteonecrosis from bisphosphonates. ADA and CDC resources confirm common side effects (dry mouth, gingivitis) and endorse preventive care. For example, ADA’s clinical guidance notes that “most classes of antihypertensive medications can cause dry mouth”, and that calcium-blockers frequently produce gingival overgrowth. A 2023 NIH-funded meta-analysis on inhaled steroids concludes they significantly raise the odds of oral candidiasis.
Our recommendations (frequent fluoride, hydration, salivary aids, dentist–physician collaboration) are grounded in these authoritative sources. The Australian Prescriber review (2016) explicitly advises informing patients about dry-mouth risk on antidepressants, conducting pre-treatment dental exams, and using “spit, don’t rinse” after fluoride application. The cancer.gov PDQ summary likewise stresses preventive dental care before chemotherapy and ongoing management of mucositis, underscoring oral complications such as dry mouth and infections. In sum, both primary research and expert guidelines support our approach: proactive oral hygiene, targeted topical therapies, and coordination of care to mitigate medication-induced oral side effects in Petersburg patients.
Frequently Asked Questions
Q: What medications commonly cause dry mouth (xerostomia)? Many drugs can reduce saliva production. These include first-generation antihistamines (diphenhydramine, chlorpheniramine), antidepressants (SSRIs like fluoxetine, SNRIs, and especially tricyclics like amitriptyline), anticholinergic medications (oxybutynin, ipratropium), antihypertensives (particularly diuretics and beta-blockers), and opioids (codeine, morphine). In practice, any patient complaining of persistent dry mouth should review their medication list for these culprits.
Q: How does medication-induced dry mouth affect my dental health? Saliva protects the teeth and gums by buffering acids and washing away debris. When saliva is low, plaque builds up faster and acids remain on teeth longer. This dramatically increases the risk of cavities and gum inflammation. Patients often crave sugar to ease dryness, compounding the decay risk. Dry mouth can also cause bad breath and soreness. In short, dry mouth is a major risk factor for tooth decay and periodontal (gum) disease.
Q: Can my medication cause my gums to bleed or grow too much? Yes. Medications that cause gingival overgrowth include calcium-channel blockers (like nifedipine) and certain anticonvulsants (phenytoin). These drugs can make gums red, swollen, and prone to bleeding. Other medications (e.g., immunosuppressants like cyclosporine) can have similar effects. Even without overgrowth, any drug that causes dry mouth can indirectly lead to gingivitis: inflamed, easily-bleeding gums. Good oral hygiene is especially important if you take these medications.
Q: How do I prevent cavities if I have a dry mouth from medication? Focus on topical fluoride and diet. Brush with fluoride toothpaste twice daily and ask your dentist about fluoride varnish or rinse at each visit. Floss daily. Avoid sugary or acidic snacks and drinks, especially between meals. Drink plenty of water or chew xylitol gum to stimulate saliva. Sealants on molars (especially for children or teens) provide extra protection. Our Petersburg clinic offers dietary counseling and sealant programs to help at-risk patients.
Q: Are there treatments to relieve medication-caused dry mouth? Yes. Chewing sugar-free gum or sucking on sugar-free candy (xylitol mints) can boost saliva flow. Use over-the-counter saliva substitutes or oral moisturizing gels. Prescription saliva stimulants (pilocarpine, cevimeline) exist for severe cases. It’s also helpful to brush more gently and often, using non-foaming toothpaste if needed. Avoid tobacco and limit alcohol or caffeine, which worsen dryness. Finally, schedule more frequent dental cleanings (every 3–4 months) so that early tooth decay or gum problems can be caught and treated.
Q: If my inhaler causes thrush, what should I do? Rinse your mouth with water or brush your teeth after each inhaler use. This simple step washes away steroid residue. Using a spacer device with metered-dose inhalers also helps. If white patches develop, your dentist or doctor can prescribe a topical antifungal mouth rinse (like nystatin). Continuing proper oral hygiene and possibly reducing inhaled steroid dose (if medically safe) will prevent recurrence.
Q: Should I stop or change my medication if it hurts my mouth? Never stop a prescribed medication without consulting your doctor. However, discuss your oral symptoms with both your dentist and physician. Often, an alternative drug or dosage adjustment can be made. For example, a different class of blood pressure medication might be tried if your current one causes severe dry mouth or gum overgrowth. Coordinated care ensures your general health needs are met without sacrificing oral health.
Q: Where can I find help in Petersburg if I have dental problems from medication? In Petersburg, Southside Dental Cares offers specialized care for dry mouth and periodontal issues. We also work with Virginia Health Department programs in the Crater District for preventive services. The Greater Richmond & Petersburg Oral Health Alliance and Mission of Mercy events sometimes provide free clinics. Ask our office for current local resources and tips on affordable care.